Dry Socket: Causes, Symptoms, Treatment & Prevention
Summary
How can you tell if the discomfort you're feeling is normal healing or a casae of dry socket after the tooth extraction? The best way is to learn about the causes and symptoms of this post-extraction complication and take the necessary steps to prevent it from happening in the first place.
Key Takeaways
- Takeaway #1: Dry socket is potential complication after a tooth extraction that occurs when the blood clot that normally forms after a tooth extraction either fails to form, dislodges, or dissolves prematurely, exposing the underlying bone and nerves and leading to pain and potential infection.
- Takeaway #2: Certain things can lead to an increased risk of dry socket, including smoking, poor oral hygiene, trauma during extraction, or not following post-extraction care instructions.
- Takeaway #3: Symptoms of dry socket can include moderate to severe pain that doesn't improve, visible bone within the extraction socket, bad breath or a foul taste in your mouth, and swelling.
- Takeaway #4: To treat dry socket, you’ll need to see your dentist. Treatment often involves cleaning the socket, placing a medicated dressing to soothe the area, and managing pain. If an infection is present, your dentist may also prescribe an antibiotic. In some cases, they may use low-level laser therapy (LLLT) to reduce pain and inflammation and promote healing.
- Takeaway #5: The best way to prevent dry socket is to follow your dentist's instructions after a tooth extraction. Instructions often include avoiding strenuous activities, refraining from smoking, maintaining a good oral hygiene routine, and eating only soft foods until the extraction wound has healed.
Table of Contents

This blog has been reviewed and approved by Dr Robert Lee, a dental professional of 35 years
LEARN MORE >Key Takeaways
What Is Dry Socket?
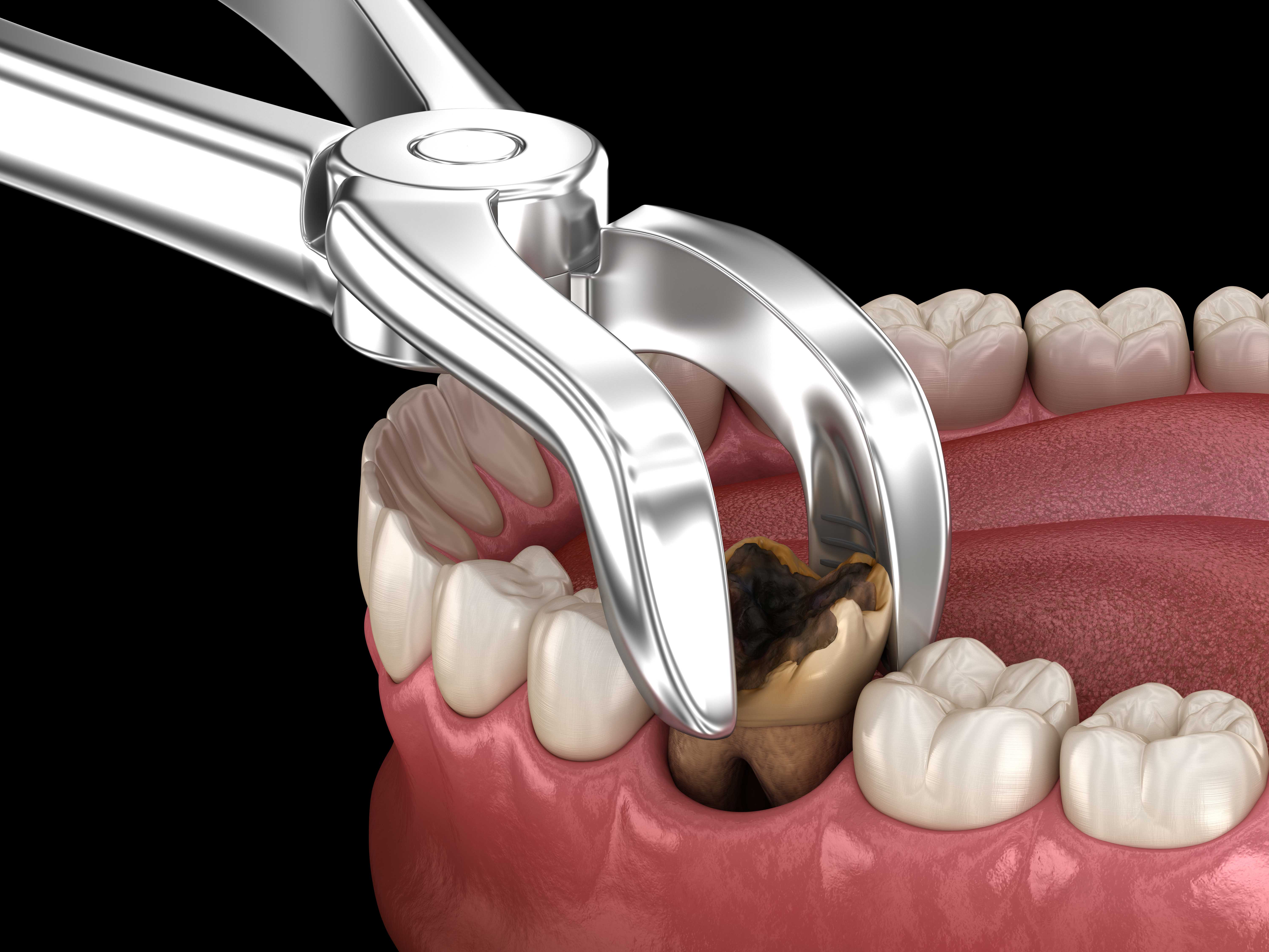
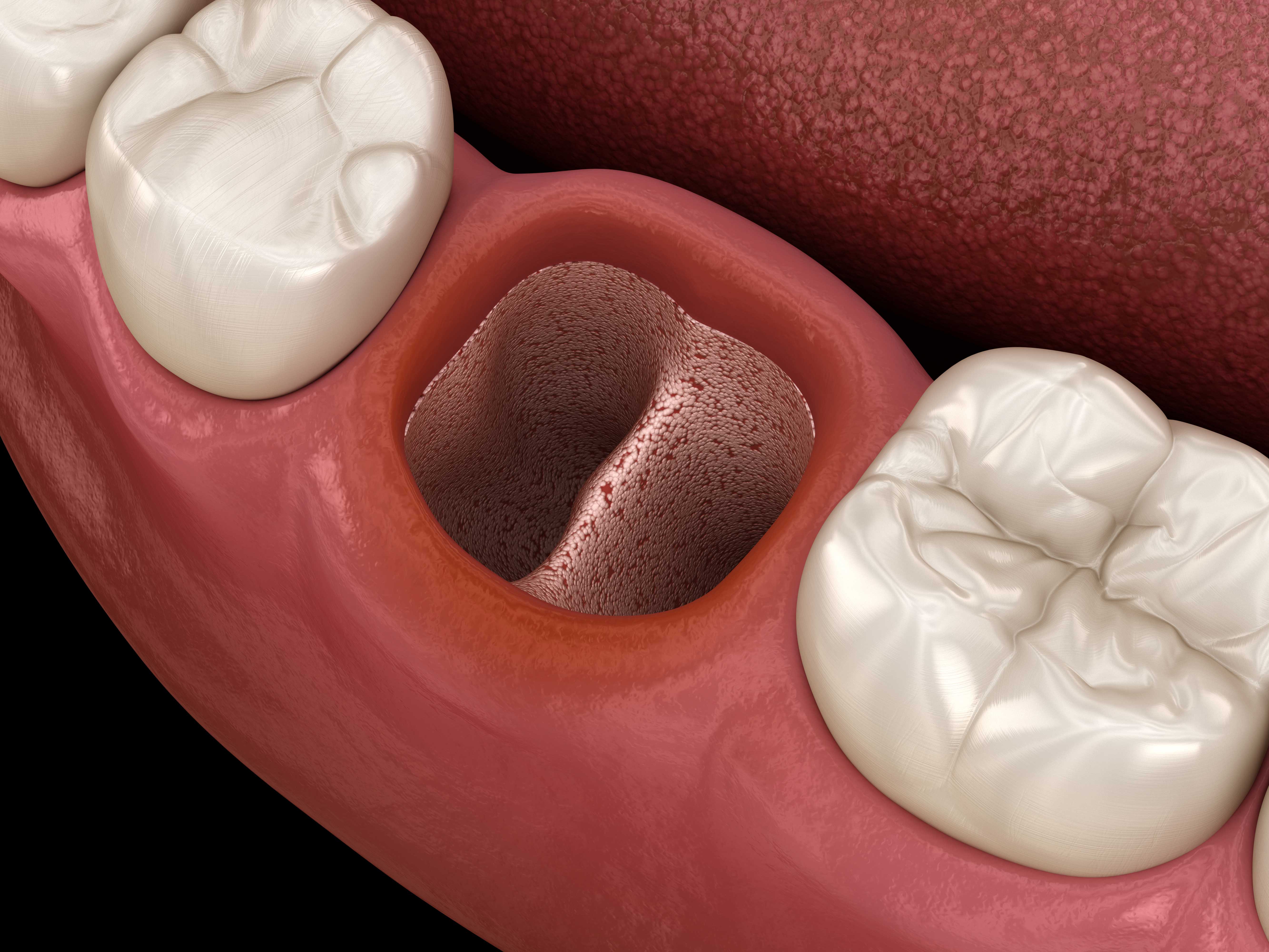
Dry socket (also known as "alveolar osteitis") is a potential complication that occurs after a tooth extraction. It happens when the blood clot that normally forms after a tooth extraction either fails to form, dislodges, or dissolves prematurely, exposing the underlying bone and nerves and leading to pain and potential infection.
Dry socket often results in moderate to severe pain, swelling, and inflammation. A bad breath or foul taste can also develop from food debris and bacteria accumulating in the open socket.
If you've just had a tooth extracted — or you're going to have one extracted in the future — you can improve the chances of avoiding dry socket by learning about its causes (and avoiding them whenever possible).
Dry Socket Causes
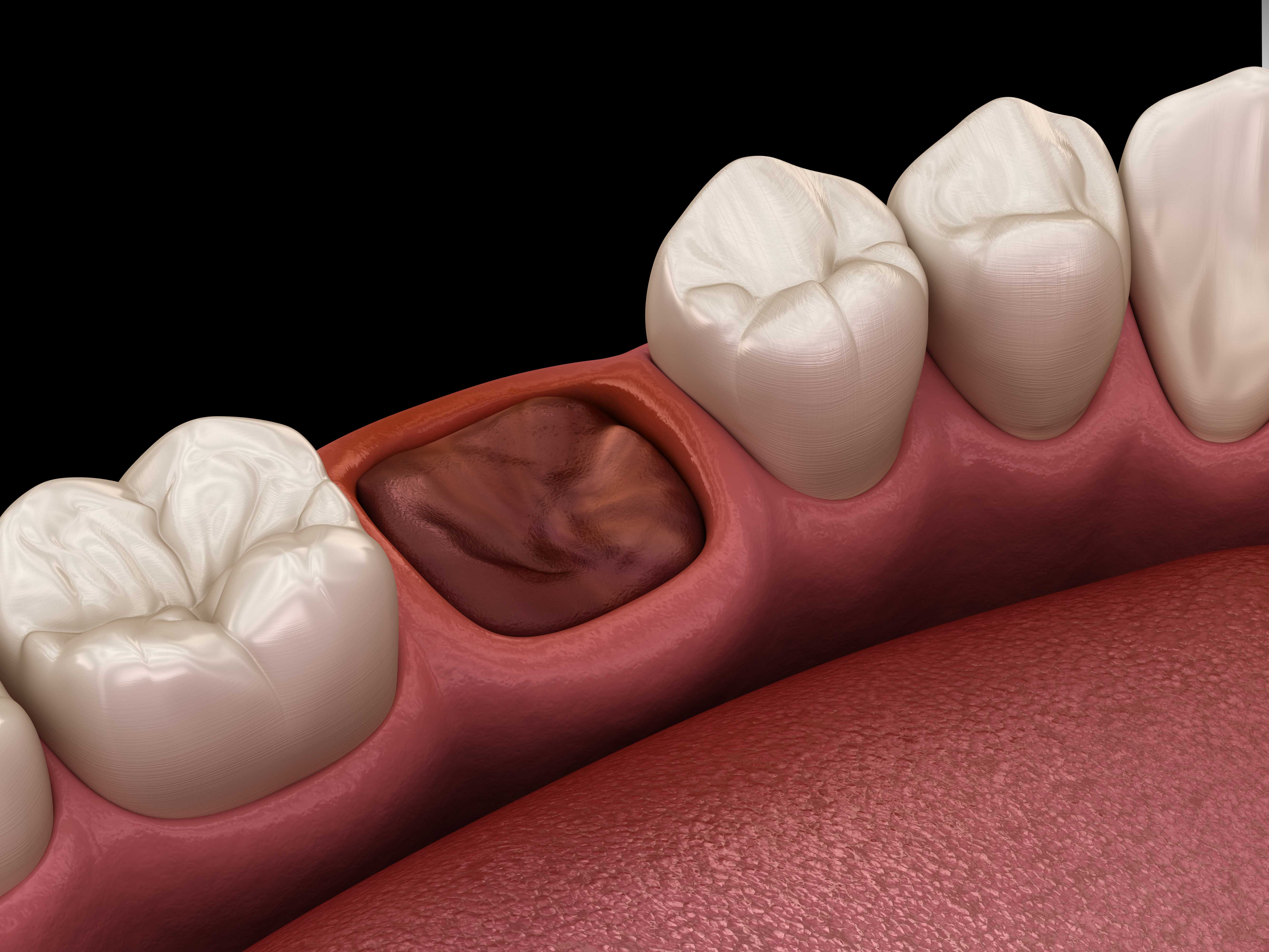
As we mentioned, dry socket happens after a tooth extraction when the blood clot that normally forms after a tooth extraction either fails to form, dislodges, or dissolves prematurely.
That said, there are a number of things that can increase your chances of this potential post-extraction complication. Avoid these behaviors after an extraction until the wound is completely healed, and your dentist gives you the all-clear.
Food and Debris
If you eat or drink right after having a tooth extracted, food debris from what you've consumed can get trapped in the empty socket and interfere with the healing process. Avoid eating hard, crunchy, or sticky foods that could dislodge the blood clot.
Be sure to ask your dentist or oral surgeon how long to wait post extraction before eating or drinking, as well as how to maintain your oral hygiene routine after having a tooth removed.
Smoking
Smoking may increase your risk of dry socket in two ways:
- The nicotine and other chemicals in tobacco products may reduce blood circulation to the area of tooth extraction and impair the healing process.
- Smoking may also impair the process by which blood fills the socket, and the suction from smoking a cigarette may also dislodge a blood clot.
Forceful Spitting or Vigorous Rinsing
Forceful spitting and vigorous rinsing can also dislodge the clot from the extraction site and lead to dry socket. The blood clot is especially susceptible to this risk in the first three to five days after your surgery.
Trauma to the Extraction Site
Trauma to the extraction site can cause the blood clot to disconnect from the surrounding tissue, leading to dry socket.
Most often, this kind of trauma happens when food debris impacts the wound site and puts pressure on the clot. Additionally, constantly probing the site with your tongue (intentionally or unintentionally) can dislodge the clot and cause further problems.
Do your best to keep everything out of that part of your mouth until the wound heals.
Dry Socket Symptoms
Dry socket symptoms can begin anywhere from two to five days after your surgery.
Intense, Throbbing Pain
A little pain after any tooth extraction surgery is to be expected, but if your pain is intense and doesn't go away, you may have dry socket.
Additionally, dry socket pain may radiate to your ear, temple, or neck and can often be more intense than during the surgery itself.
Empty Socket or Visible Bone
One of the best ways to identify a dry socket is to look at the wound itself. If you don't see a dark red blood clot or if you notice visible bone, visit your dentist right away before the problem worsens.
Bad Breath or Taste in Your Mouth
When the socket is exposed, food particles and bacteria can collect in the area. This can lead to a foul smell or bad taste in your mouth.
Swelling and Inflammation
The tissue around the wound site will naturally swell and become inflamed, but if this inflammation is accompanied by intense pain that doesn't get better in a few days, you may be at risk of dry socket. See your dentist right away.
Even if you think you have symptoms of dry socket — and it turns out that you don't — there's no shame in visiting a dentist. It's much better to be safe than sorry when it comes to this painful post-extraction complication.
Dry Socket Treatment
If your dentist confirms that you have dry socket, treatment will typically involve the following:
- Your dentist or oral surgeon will flush the socket with saline or an antiseptic solution to remove any food particles, debris, or bacteria that may be contributing to the pain and inflammation.
- They'll pack the socket with a medicated dressing that relieves pain and promotes healing.
- They may prescribe pain relief medication to help manage the pain if needed.
- If an infection is present, they may prescribe antibiotics to eliminate the bacteria and resolve the infection.
- They'll schedule a number of checkups to make sure everything is healing nicely. The dressing may need to be changed every few days, depending on the severity of the pain and the healing progress.
In addition to this common treatment, some dentists will use low-level laser therapy (LLLT) to reduce the pain and inflammation and help your wound heal.
Dry Socket Prevention
The best thing you can do to prevent dry socket is to follow your dentist's instructions. This may include such steps as:
- Avoiding strenuous activity.
- Refraining from smoking for at least a week after (more is better and quitting altogether is best).
- Gently maintaining your oral hygiene routine. Your dentist will provide specific instructions, which often include gently brushing and flossing other areas of your mouth while completely avoiding the extraction site for the first day or so. They may also recommend gentle rinsing with a prescribed or saltwater mouth rinse after a specific period.
- Eating soft foods for a week after the surgery.
Again, be sure to talk to your dentist or oral surgeon about recommendations to prevent dry socket. They may have you alter your oral hygiene routine slightly (depending on your individual case) and make some other suggestions to help you heal faster.
Keep Your Mouth Clean with Oral-B

You may not be able to avoid certain tooth extractions, such as having your wisdom teeth removed, but you can prevent other dental issues that lead to tooth extraction by maintaining a good oral hygiene routine.
The Oral-B iO Electric Toothbrush Series can help. It removes 100% more plaque than a manual toothbrush for a professional clean feeling every day. The iO9’s Gentle Care mode is also perfect for sensitive areas.
For a complete and powerful routine, use a Crest toothpaste with stannous fluoride like Crest Pro-Health, floss at least once a day with Oral-B Glide floss, and rinse with a Crest Pro-Health mouthwash.
FAQs
-
Dry socket vs. normal: What's the difference?
-
When can I stop worrying about getting dry socket?
-
What does dry socket feel like?
Sources
- https://www.mayoclinic.org/diseases-conditions/dry-socket/symptoms-causes/syc-20354376
- https://my.clevelandclinic.org/health/diseases/ 17731-dry-socket
- https://medlineplus.gov/ency/patientinstructions/ 000780.htm
- https://pmc.ncbi.nlm.nih.gov/articles/ PMC5932271/
- Adam R. (2020). Introducing the Oral-B iO electric toothbrush: next generation oscillating-rotating technology. International Dental Journal, 70 Suppl 1(Suppl 1), S1–S6. https://doi.org/10.1111/idj.12570
- Biesbrock, A., et al. (2019). The effects of bioavailable gluconate chelated stannous fluoride dentifrice on gingival bleeding: Meta-analysis of eighteen randomized controlled trials. Journal of Clinical Periodontology, 46(12), 1205–1216. https://doi.org/10.1111/jcpe.13203
- Mankodi, S., et al. (2005). A 6-month clinical trial to study the effects of a cetylpyridinium chloride mouthrinse on gingivitis and plaque. American Journal of Dentistry, 18 Spec No, 9A–14A. https://pubmed.ncbi.nlm.nih.gov/16178130/
- Terézhalmy, G. T., et al. (2008). Plaque-removal efficacy of four types of dental floss. Journal of Periodontology, 79(2), 245–251. https://doi.org/10.1902/jop.2008.070345
- Zou, Y., et al. (2024). A meta-analysis comparing toothbrush technologies on gingivitis and plaque. International Dental Journal, 74(1), 146-156. https://doi.org/10.1016/j.identj.2023.06.009
Table of Contents
- What Is Dry Socket?
- Dry Socket Causes
- Dry Socket Symptoms
- Dry Socket Treatment
- Dry Socket Prevention
- Keep Your Mouth Clean with Oral-B
-
- FAQs
- Sources

This blog has been reviewed and approved by Dr Robert Lee, a dental professional of 35 years
LEARN MORE >
Send Tips
for oral care tips, expert advise, and exclusive offers.

Send Tips
for oral care tips, expert advise, and exclusive offers.


